
IVF (In Vitro Fertilisation) is a process in which a woman's eggs are fertilised with sperm outside the body in a laboratory, and the resulting embryo is transferred into the uterus to establish a pregnancy. A single IVF cycle in India takes 14 to 21 days, with the full process from first consultation to embryo transfer typically spanning 6 to 8 weeks.
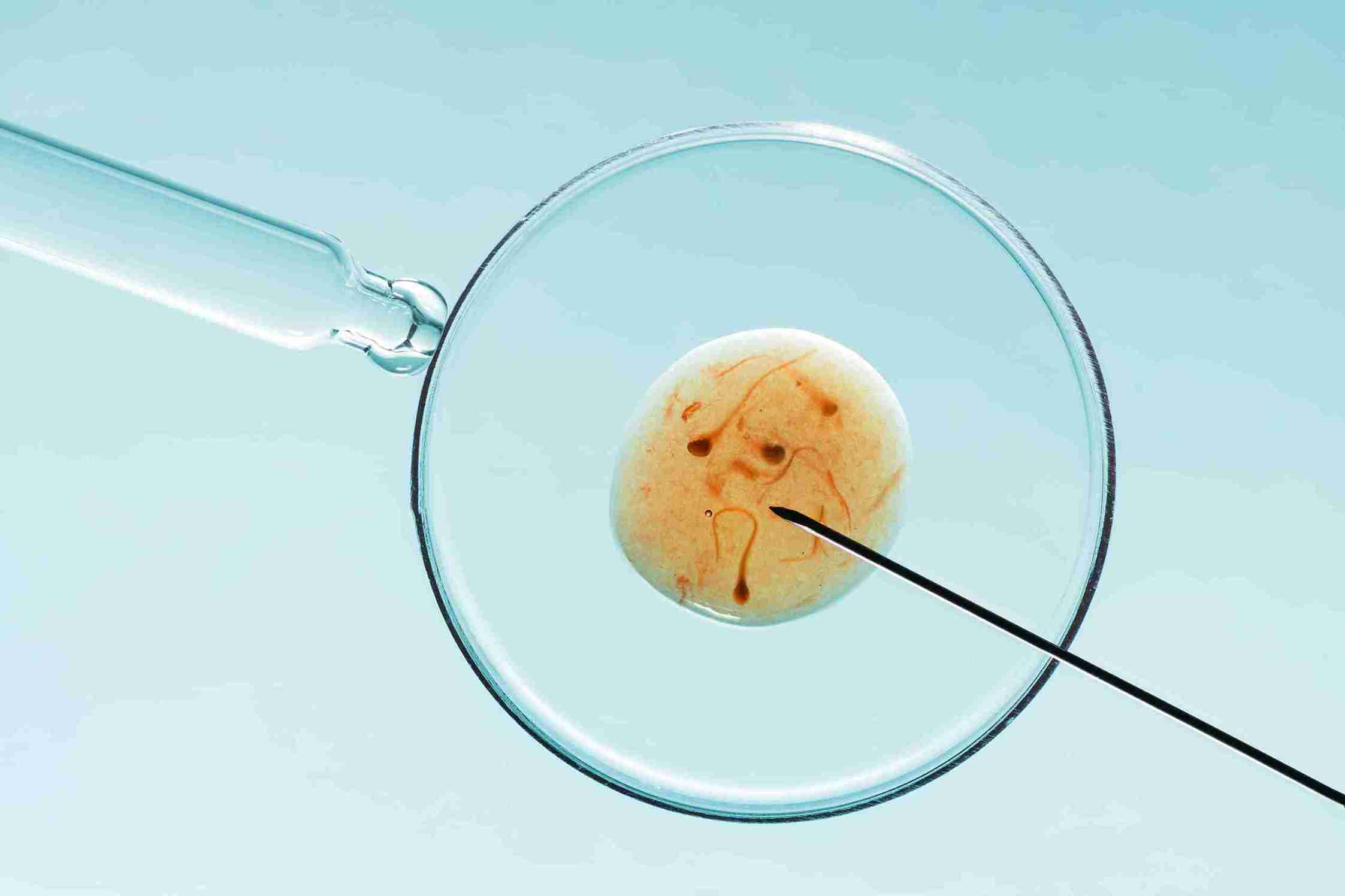
IVF stands for In Vitro Fertilisation from the Latin in vitro, meaning 'in glass.' It is an assisted reproductive technology (ART) in which eggs are retrieved from a woman's ovaries, fertilised with sperm in a controlled laboratory environment, and the best-quality embryo is transferred back into the uterus. IVF bypasses the need for the fallopian tubes and enables fertilisation to occur under precise, monitored conditions, significantly increasing the chance of conception for couples who cannot conceive naturally.
Key facts at a glance:
India performs approximately 2 to 2.5 lakh IVF cycles annually, a number that has grown sharply as awareness and acceptance of assisted reproduction increase. With 1 in 6 Indian couples estimated to face infertility at some point driven by delayed marriages, PCOS, endometriosis, and rising male factor infertility IVF has become a critical pathway to parenthood. Yet misinformation about the process, the pain involved, and realistic success rates causes many couples to delay seeking help. Understanding what IVF actually involves, step by step , allows couples to make informed, timely decisions rather than spending years on treatments unlikely to succeed in their specific situation.
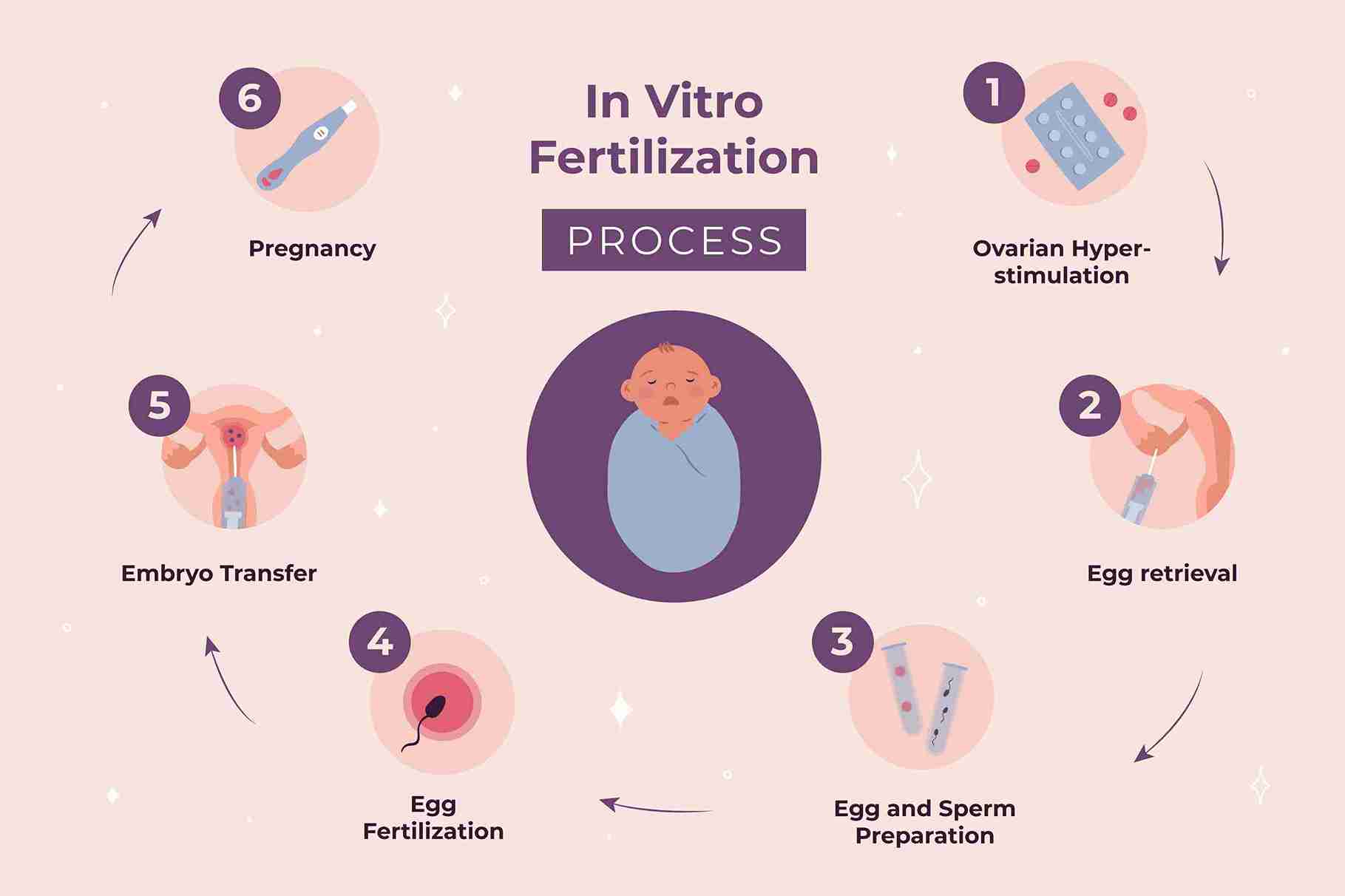
IVF is not a single procedure, it is a structured sequence of seven stages, each building on the last. Your fertility specialist may modify the protocol based on your ovarian reserve, age, diagnosis, and response to medication.
Before any treatment begins, both partners undergo a comprehensive fertility evaluation. For women, this includes blood tests for AMH, FSH, LH, and estradiol, along with a transvaginal ultrasound to count antral follicles and assess the uterine cavity. For men, a semen analysis evaluates sperm count, motility, and morphology. Infectious disease screening (HIV, Hepatitis B, and C) is mandatory for both partners under ICMR guidelines. Based on these results, the fertility specialist designs a personalised treatment protocol and discusses realistic expectations, cost, and likely number of cycles needed.
The ovaries are stimulated using injectable gonadotropins, typically FSH or a combination of FSH and LH, taken daily for 8 to 14 days. Normally, the body produces one egg per menstrual cycle. Stimulation encourages multiple follicles to mature simultaneously, increasing the number of eggs available for fertilisation. During this phase, the patient visits the clinic every 2 to 3 days for blood tests and ultrasound scans to monitor follicular growth and adjust medication doses accordingly. When the leading follicles reach 18 to 20 mm in diameter, the trigger shot is administered.
Exactly 36 hours before egg retrieval, a trigger injection of hCG (human chorionic gonadotropin) is administered to complete final egg maturation. Egg retrieval is performed under intravenous sedation, so the patient is comfortable and pain-free throughout. A thin needle is guided through the vaginal wall into each ovary under ultrasound vision, and follicular fluid containing the eggs is aspirated. The procedure takes 15 to 25 minutes. Mild cramping and spotting for a day or two afterward are normal. Patients return home the same day.
On the same day as egg retrieval, the male partner provides a semen sample, which is processed in the lab to isolate the healthiest, most motile sperm. Fertilisation occurs in one of two ways. In conventional IVF, approximately 50,000 sperm are placed in a dish with each mature egg. In ICSI (Intracytoplasmic Sperm Injection), a single healthy sperm is injected directly into each egg, recommended when sperm quality is significantly impaired. Fertilisation is confirmed the following morning. Typically, 60 to 80% of mature eggs fertilise successfully.
Fertilised eggs are kept in a time-lapse incubator in the IVF laboratory, where conditions mimic the human body. The embryologist monitors development daily. A 2-cell embryo on Day 1, a 4-cell embryo on Day 2, and a blastocyst (80-120 cells) by Day 5 is the ideal trajectory. Most Indian clinics now prefer blastocyst transfer on Day 5 over Day 3 transfer because blastocysts have proven developmental potential and a higher implantation rate. If Preimplantation Genetic Testing (PGT) is recommended, a biopsy of 5 to 8 cells is taken from the blastocyst at this stage.
Embryo transfer is the simplest stage of the IVF process. The selected embryo is loaded into a thin, flexible catheter, which is passed gently through the cervix into the uterine cavity under ultrasound guidance. No sedation is required. The procedure takes 5 to 10 minutes and feels similar to a routine gynaecological examination. The patient rests briefly in the clinic and can return to light daily activity the same day. Complete bed rest after transfer is not medically recommended and does not improve outcomes. Progesterone support is prescribed to prepare the uterine lining for implantation.
After embryo transfer, the patient waits approximately 10 to 14 days before a beta-hCG blood test confirms whether implantation has occurred. If the result is positive, a second beta-hCG test is done 48 hours later to confirm rising hormone levels, followed by an ultrasound at 6 to 7 weeks to detect the foetal heartbeat. If the result is negative, the fertility team will review the cycle and discuss whether a frozen embryo transfer (FET) or a new stimulation cycle is the appropriate next step.
_11zon.jpg)
IVF is recommended when other, less invasive treatments such as IUI or ovulation induction have failed, or when a diagnosis makes natural conception highly unlikely. The most common indications seen in Indian fertility clinics are:
• Blocked or damaged fallopian tubes: The most common structural cause of female infertility in India, often resulting from pelvic inflammatory disease, prior infections, or previous surgery. IVF bypasses the tubes entirely, making this a strong indication.
• PCOS (Polycystic Ovary Syndrome): Affects up to 20% of Indian women of reproductive age. Irregular or absent ovulation makes natural conception difficult; IVF with controlled stimulation produces multiple eggs in a single cycle.
• Low sperm count or motility (male factor infertility): Responsible for 30-40% of infertility cases in India. ICSI within an IVF cycle allows fertilisation with as few as a single viable sperm, making severe male factor cases treatable.
• Endometriosis: Scar tissue and endometrial lesions reduce egg quality, damage tube function, and impair implantation. IVF with careful embryo selection significantly improves outcomes compared to natural conception.
• Diminished ovarian reserve (low AMH or low antral follicle count): Found in women over 35 or those who have had ovarian surgery. IVF maximises egg collection in a single stimulated cycle, preserving what reserve remains.
• Unexplained infertility: When all standard tests return normal results but conception does not occur after 12 months of trying. IVF with ICSI often reveals fertilisation defects that standard testing cannot detect.
• Genetic carrier conditions: Couples who carry hereditary disorders such as thalassaemia or chromosomal translocations require IVF combined with PGT to ensure only unaffected embryos are transferred.
IVF outcomes are influenced by both clinical factors and lifestyle choices. The steps below are evidence-backed actions specific to the Indian context that improve embryo quality, uterine receptivity, and overall cycle outcomes.
• Start CoQ10 (600 mg/day) 3 months before IVF: Coenzyme Q10 improves mitochondrial function in eggs, directly enhancing embryo quality, especially relevant for women over 35 or those with low ovarian reserve.
• Eat 80g of protein daily from dal, paneer, eggs, and lean meat: Adequate protein supports follicular development during ovarian stimulation and improves egg maturity rates.
• Correct vitamin D deficiency (supplement with 2,000-4,000 IU/day if below 30 ng/mL): Vitamin D deficiency is extremely common in urban India and is independently associated with lower IVF implantation rates.
• Eliminate tobacco and limit alcohol to zero: Both partners should stop smoking at least 3 months before beginning IVF. Smoking reduces ovarian reserve and damages sperm DNA integrity.
• Walk 30 minutes daily, but avoid intense exercise: Moderate activity supports circulation and reduces cortisol; high-intensity training during stimulation increases the risk of ovarian hyperstimulation syndrome (OHSS).
• Request blastocyst transfer (Day 5) over Day 3 cleavage transfer: Blastocysts have a higher implantation rate because only developmentally competent embryos reach Day 5. Ask your clinic specifically about their blastocyst culture rate.
• Consider PGT-A if over 37 or after 2 failed cycles: Preimplantation Genetic Testing for Aneuploidy screens embryos for chromosomal abnormalities before transfer, reducing failed implantation and miscarriage risk.
• Ask about ERA (Endometrial Receptivity Analysis) after recurrent failure: ERA identifies the precise implantation window for your uterus, a single biopsy that can explain why transfers repeatedly fail in women with good-quality embryos.
• Use frozen embryo transfer (FET) if OHSS risk is identified: Freezing all embryos and performing transfer in a subsequent natural cycle is safer and often gives better implantation rates than a fresh transfer in a stimulated cycle.
The most common mistake Indian couples make is waiting too long before consulting a specialist. Use the decision table below to determine when to act:
If you are in Gurgaon, Delhi NCR, or anywhere across India and have been trying to conceive for more than six months without success, book a fertility consultation today. Early assessment costs nothing and prevents years of unnecessary delay.

IVF success rates in India have improved consistently over the past decade, driven by advanced embryology laboratories, blastocyst culture, and AI-assisted embryo selection. Maternal age remains the single strongest predictor of outcome. The table below reflects live birth rates per cycle from ICMR-accredited fertility centres and ASRM 2023 guidelines:
Source: ICMR-registered clinic outcome data 2024; ASRM Guidelines 2023; Dr. Sowjanya Aggarwal IVF Success Rate Analysis, March 2026.
Cumulative success rates across 3 cycles for women under 35 can reach 60 to 80%, which is why fertility specialists recommend planning for multiple cycles from the outset. Donor egg IVF consistently delivers 60 to 70% success regardless of the recipient's age, making it the recommended path for women over 42 or those with severely diminished ovarian reserve.
The IVF process is not significantly painful, though some stages involve mild discomfort. The daily hormone injections during ovarian stimulation feel like a routine subcutaneous injection; most patients administer these themselves at home after brief training. Egg retrieval is performed under intravenous sedation, so no pain is felt during the procedure. Some women experience mild cramping and bloating for a day or two afterward, similar to menstrual discomfort. Embryo transfer requires no anaesthesia and is comparable in sensation to a cervical smear test.
A single IVF cycle from the start of ovarian stimulation to embryo transfer takes approximately 14 to 21 days. The full journey from first consultation to transfer, including diagnostic testing and protocol planning, typically spans 6 to 8 weeks. The two-week wait after embryo transfer adds another 10 to 14 days before a pregnancy test result is available. If a frozen embryo transfer (FET) is planned instead of a fresh transfer, there is usually a gap of 4 to 6 weeks between the retrieval cycle and the transfer cycle.
IVF and ICSI differ only at the point of fertilisation. In conventional IVF, eggs and sperm are placed together in a dish, and fertilisation occurs naturally. In ICSI (Intracytoplasmic Sperm Injection), a single sperm is injected directly into each egg using a fine needle under a high-powered microscope. ICSI is recommended when sperm count or motility is below normal, when previous IVF cycles showed poor fertilisation, or when sperm is retrieved surgically in cases of azoospermia. ICSI does not automatically produce better outcomes when sperm parameters are normal; the decision should be made based on your specific semen analysis results.
There is no universal answer, as the number of cycles depends on age, diagnosis, embryo quality, and uterine response. Among women under 35, approximately 40 to 45% conceive on the first cycle. Across three cumulative cycles, this rises to 65 to 80%. Your fertility specialist will review your response after each cycle and adjust the protocol accordingly. Couples should discuss a multi-cycle plan at the outset, both financially and emotionally, rather than approaching IVF one cycle at a time without a broader strategy.